


Security policy (edit with Customer reassurance module)

Delivery policy (edit with Customer reassurance module)

Return policy (edit with Customer reassurance module)
Pharmacodynamics
Local anesthetic with moderate anesthetic activity and a wide breadth of therapeutic action. Being a weak base, it blocks Na + channels, interferes with the generation of impulses at the ends of sensory nerves and conduction of impulses along the nerve fibers. Changes the action potential in the membranes of nerve cells without a pronounced effect on the resting potential. Suppresses the holding of not only pain, but also pulses of another modality. With absorption and direct vascular injection into the blood stream, it reduces the excitability of peripheral cholinergic systems, reduces the formation and release of acetylcholine from preganglionic endings (it has some ganglion-blocking action), eliminates smooth muscle spasm, reduces the excitability of the myocardium and motor cortex. When administered intravenously, it has an analgesic, hypotensive and antiarrhythmic effect (it increases the effective refractory period, reduces anxiety, automatism and conductivity), and in large doses it can disturb the neuro-minor conductivity. Eliminates the downward inhibitory effects of the reticular formation of the brain stem. Inhibits polysynaptic reflexes. In large doses, it can cause convulsions.It has a short anesthetic activity (the duration of infiltration anesthesia is 0.5-1 h).
Pharmacokinetics
Subject to complete systemic absorption. The degree of absorption depends on the place and route of administration (especially on vascularization and blood flow velocity in the area of administration) and the final dose (amount and concentration). It is rapidly hydrolyzed by plasma and liver esterases to form 2 main pharmacologically active metabolites: diethylaminoethanol (it has a moderate vasodilating effect) and para-aminobenzoic acid (it is a competitive antagonist of sulfanilamide Chemotherapy drugs and can weaken their antimicrobial effect). The half-life is 30-50 seconds, in the neonatal period 54-114 s. It is excreted mainly by the kidneys as metabolites, and no more than 2% is excreted unchanged.
Indications for use
Contraindications
Hypersensitivity (including para-aminobenzoic acid and other local anesthetics), children under 12 years of age. Pronounced fibrous changes in the tissues (for anesthesia by creeping infiltration).
Carefully
Emergency surgery, accompanied by acute blood loss, conditions, accompanied by a decrease in hepatic blood flow (for example, in CNS, liver disease),progression of cardiovascular insufficiency (usually due to the development of heart block and shock), inflammatory diseases or infected injection sites, pseudocholinesterase deficiency, renal failure, children age (from 12 to 18 years), in elderly patients (over 65), debilitated patients, pregnancy, childbirth period.
Dosage and administration
For infiltration anesthesia, use solutions of 2.5 mg / ml, 5 mg / ml; for anesthesia by the method of Vishnevsky (tight creeping infiltration) - solutions of 1.25 mg / ml, 2.5 mg / ml. To reduce the absorption and prolong the action under local anesthesia, a 0.1% solution of epinephrine hydrochloride is added in 1 drop per 2-5-10 ml of procaine solution.
In case of perirenal blockade (according to AV Vishnevsky), 50-80 ml of a solution of 5 mg / ml or 100-150 ml of a solution of 2.5 mg / ml are injected into the perrenal cellulose tissue.
When vagosympathetic blockade 30-100 ml of a solution of 2.5 mg / ml is administered.
For the circular and paravertebral blockade, a solution of 2.5 mg / ml or 5 mg / ml is injected intradermally.
Higher doses for infiltration anesthesia for adults: the first single dose at the beginning of the operation is no more than 500 ml of a solution of 2.5 mg / ml or 150 ml of a solution of 5 mg / ml.
The maximum dose for use in children up to 15 mg / kg.
Side effect
Headache, dizziness, drowsiness, weakness, increase or decrease in blood pressure, collapse, peripheral vasodilation, bradycardia, arrhythmia, pain in a difficult cell, trizm, tremor, impaired vision and hearing, nystagmus, persistent anesthesia, hypothermia, methemoglobinemia, allergies, allergies, persistent anesthesia, hypothermia, methemoglobinemia, allergies, allergies, nystagmus, persistent anesthesia, hypothermia up to anaphylactic shock).
Overdose
Symptoms: pallor of the skin and mucous membranes, dizziness, nausea, vomiting, "cold" sweat, increased respiration, tachycardia, lowering blood pressure until collapse, apnea, methemoglobinemia. The effect on the central nervous system is manifested by a sense of fear, hallucinations, convulsions, motor agitation.
Treatment: maintaining adequate pulmonary ventilation, detoxification and symptomatic therapy.
Interaction
Strengthens the inhibitory effect on the central nervous system of general anesthetic drugs, hypnotics and sedatives, narcotic analgesics and tranquilizers.
Anticoagulants (ardeparin, dalteparin, danaparoid, enoxaparin, Heparin, warfarin) increase the risk of bleeding.
When processing the injection site of a local anesthetic with disinfectant solutions containing heavy metals, the risk of developing a local reaction in the form of pain and swelling increases.
Use with MAO inhibitors (furazolidone, procarbazine, selegilin) increases the risk of hypotension.
Strengthen and lengthen the action of muscle relaxants.
When procaine is prescribed together with narcotic analgesics, an additive effect is noted, which is used during spinal and epidural anesthesia, while respiratory depression is enhanced.
Vasoconstrictors (epinephrine, methoxamine, phenylephrine) prolong the local anesthetic effect.
Procaine reduces the anti-myasthenic effect of drugs, especially when used in high doses, which requires an additional correction for the treatment of myasthenia.
Cholinesterase inhibitors (antimyasthenic drugs, cyclophosphamide, demecarin, ecothiophate, thiotepa) reduce the metabolism of procaine.
Metabolite procaine (para-aminobenzoic acid) is an antagonist of sulfonamides.
special instructions
Patients are required to monitor the functions of the cardiovascular, respiratory and central nervous systems. It is necessary to cancel MAO inhibitors 10 days before the introduction of a local anesthetic. During the period of treatment, it is necessary to refrain from driving vehicles and engaging in potentially hazardous activities that require high concentration of attention and quickness of psychomotor reactions. Before use, mandatory testing of individual sensitivity to the drug. It should be borne in mind that when conducting local anesthesia when using the same total dose, the toxicity of Novocaine is the higher, the more concentrated the solution is used. Not absorbed from mucous membranes; does not provide surface anesthesia for skin use.
Release form
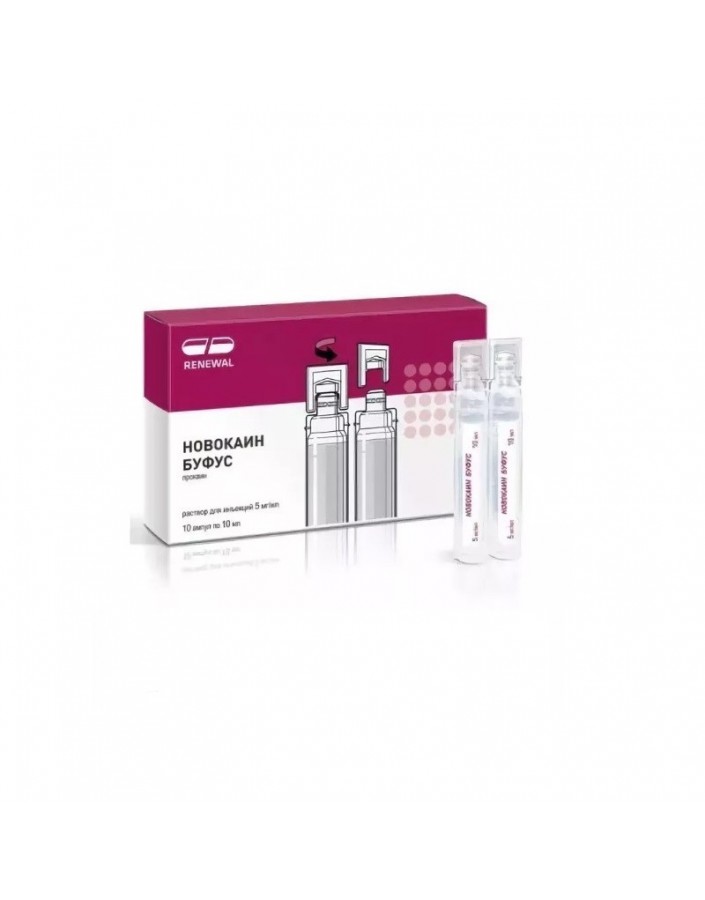
Solution for injection 5 mg / ml.
On 5 ml, 10 ml in ampoules of neutral glass, or in polymer ampoules, from high-density polyethylene, or from low-pressure polyethylene, or from polyethylene for medical purposes, or from polyethylene, or polypropylene for infusion solutions and injectables.
On 10 ampoules of neutral glass with the instruction for application are placed in a box from a cardboard for a consumer container with a corrugated insert from paper pack. In each box they put an ampoule knife or a scarifier.When packaging ampoules with notches, rings and dots, ampoule knives or scarifiers do not insert. On 10 ampoules polymeric with the instruction for application are placed in a pack from a cardboard for a consumer container.
Storage conditions
List B. In the dark spot.
Keep out of the reach of children.